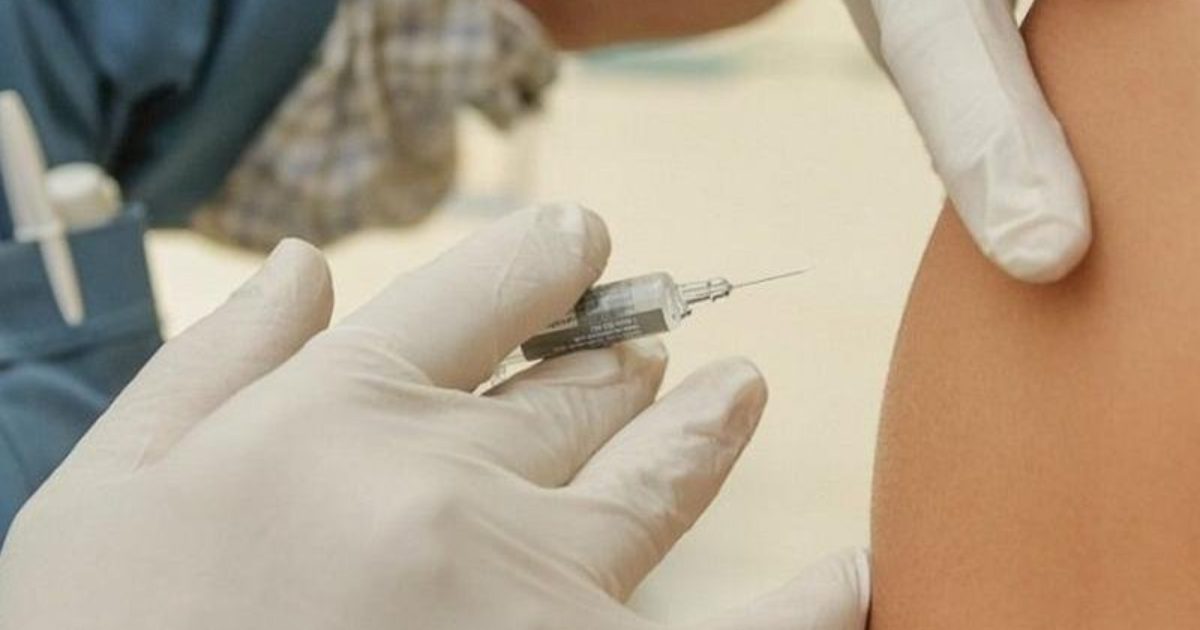
The experimental COVID-19 shots were the first mRNA ‘vaccines’ to be rolled out on a massive scale.
“Pfizer’s COVID-19 vaccine is the first mRNA product to achieve full FDA approval in the U.S.,” Johns Hopkins stated.
Johns Hopkins explained some of the ‘advances’ utilized to develop mRNA injections:
The early years of mRNA research were marked by a lot of enthusiasm for the technology but some difficult technical challenges that took a great deal of innovation to overcome.
The biggest challenge was that mRNA would be taken up by the body and quickly degraded before it could “deliver” its message—the RNA transcript—and be read into proteins in the cells.
The solution to this problem came from advances in nanotechnology: the development of fatty droplets (lipid nanoparticles) that wrapped the mRNA like a bubble, which allowed entry into the cells. Once inside the cell, the mRNA message could be translated into proteins, like the spike protein of SARS-CoV-2, and the immune system would then be primed to recognize the foreign protein.
These ‘technological advances’ have decimated human health.
Check out these prior reports for more info:
(WATCH) Dr. Naomi Wolf Discusses Pfizer COVID-19 Jab Documents and How It Compares to Genocide
Pfizer and Moderna’s mRNA technology to develop the COVID-19 gene therapies has been a medical disaster.
Yet, pharmaceutical manufacturers are set to use this dangerous technology to create new influenza ‘vaccines.’
Via Johns Hopkins:
Already, vaccine manufacturers are developing mRNA vaccines to protect against other respiratory viruses such as the flu. Moderna is exploring applications of the technology to protect against HIV. It’s a new era for vaccine technology and production, and a testament to scientific progress and decades of research.
TIME added:
Both Moderna and Pfizer—makers of the first vaccines to earn U.S. Food and Drug Administration (FDA) approval using the mRNA technology—are studying whether subbing in the influenza virus’ genetic material in that platform will prove equally fruitful.
On Sept. 14, Pfizer announced that the first volunteers had received doses of its mRNA flu shot; the Phase 3 study will involve more than 25,000 adults in the U.S. ages 18 and up who will be randomly assigned to receive either the experimental vaccine or a placebo. In June, Moderna announced its late-stage trial of an mRNA-based influenza vaccine that targets the same flu strains that are expected to circulate this fall and winter. Moderna’s study will involve 6,000 adults in the U.S. and other countries in the southern hemisphere, which experiences its flu season several months before the U.S. Both trials are now at similar stages; neither company has provided a timeline for when they might expect results, and, if those results are positive, when they might submit a request to the FDA for approval.
Public health experts are hoping it won’t be long, however. The advantage of the mRNA platform is that it’s flexible and generalizable. Theoretically, scientists only need to switch out the genetic material, or mRNA sequences, from one virus for another. It’s a matter of figuring out which specific genes will activate the immune system the best—and that’s where researchers have decades of experience with influenza that they didn’t have with SARS-CoV-2.

Join the conversation!
Please share your thoughts about this article below. We value your opinions, and would love to see you add to the discussion!